What is Postherpetic Neuralgia (PHN)?
Postherpetic Neuralgia (PHN) – Complication of Shingles
The pain of shingles lasts on average about 4-5 weeks. Any continuation of pain beyond this time is considered Post Herpetic Neuralgia, and is referred to as PHN.
If this describes you, a friend or a loved one,
Please read on…
In general, 1 out every 5 people who have shingles, will go on to suffer with PHN. This ratio varies widely however, depending on your age.
If younger than 40, Post Herpetic Neuralgia (PHN) rarely develops, unless your immune system is compromised. The immunocompromised are those whose immune systems are weakened by a disease such as AIDS, by drugs used to suppress the rejection of a transplanted organ, or by radiation or chemotherapy for cancer.
Other things that could compromise your immune system at this age are heredity, stress and chronic disorders such as chronic pulmonary, cardiovascular, hepatic, hematological, neurologic, neuromuscular, or metabolic disorders.
By age 60, your risk of PHN rises to 50%, and at age 70 it reaches 75%. In short, the older you are when you develop shingles, the more likely you are to suffer with PHN afterward.
Even though there is no way to predict how long PHN will last or how severe it will be, or even who will develop Postherpetic Neuralgia (PHN). PHN seems to develop most however, in those who suffered severe shingles symptoms, or experience severe pain before the shingles rash appeared. Also, location of the infection seems to have some bearing on the severity and length of PHN.
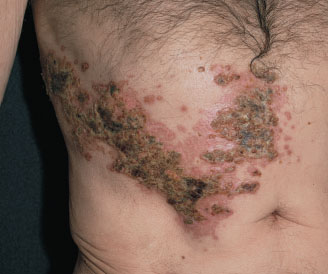
Postherpetic Neuralgia (PHN) of the Trunk
Dermatome refers to the area of skin that is supplied by a single nerve fiber from a single dorsal root.
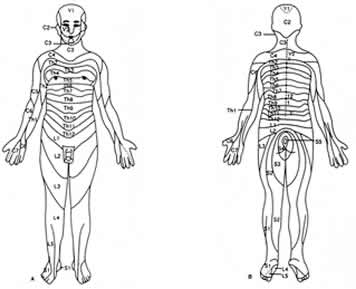
When you have shingles, it can appear most often on various areas of the trunk, especially close to your waist. Shingles, and subsequently PHN is usually confined to a single dermatome, or at least 2 or 3 adjacent ones. (This area will be covered at length in upcoming reports).
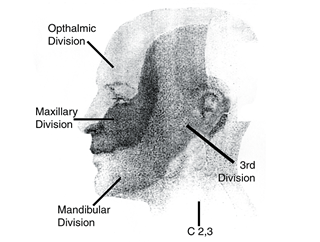
Postherpetic Neuralgia (PHN) of the Face and Scalp
The rate of occurrence of PHN is greater for those with shingles on the face and scalp. In fact it accounts for about 15% of all cases.
Pain from Post Herpetic Neuralgia (PHN) in this area seems more severe. A potentially serious problem could develop if the virus spreads to you eye. This is referred to as Herpes Zoster Ophthalmicus or HZO. With shingles in this area, it is best to include an ophthalmologist in your treatment.
Postherpetic Neuralgia (PHN) of the Extremities
As mentioned earlier, shingles and subsequently PHN is most common on the trunk and buttocks, but it can also occur on arms and legs if the nerves to these areas are affected. (This area will be covered at length in upcoming reports).
Ramsay Hunt Syndrome
It is very unusual for shingles to develop in the facial nerve. When this happens, the pain-sensing trigeminal nerve, and the acoustic nerve, which registers sensations of hearing and balance in the inner ear, can become affected.
When this happens, the results are known as Ramsay Hunt syndrome, and produce the following symptoms:
A shingles rash that develops on or near the ear, in the ear canal, as well as on the mouth, face, neck and scalp. This is associated with severe earache, pain in the mastoid bone (the bone behind the ear), partial loss of hearing, and inner ear disturbances resulting in dizziness (vertigo), nausea, and sometimes tinnitus (abnormal sounds). There is also loss of taste in part of the tongue, and paralysis of the facial muscles.
Some of these symptoms may resolve once the acute infection has passed, but the hearing loss and facial paralysis may last for months.
There is a slightly higher incidence of Ramsay Hunt Syndrome in women than men, and the overall incidence is higher after the age of fifty.
The treatment of Ramsay Hunt Syndrome is mostly symptomatic, and all patients show some degree of recovery. Maximum recovery usually occurs in 6 – 12 months.
Other terms used to describe the Ramsay Hunt Syndrome are – herpes zoster cephalicus, herpes zoster oticus, and herpes zoster auricularis.
Allodynia
Allodynia is a spasm of stabbing pain triggered by some other sensation that is not in itself painful. A simple light, moving touch across the skin such as friction from clothing, or a light breeze can trigger the pain.
Just wearing a shirt can set off awful stabs of pain. Other potential triggers of allodynia are heat, cold and sunlight. How this happens is not well understood, but these harmless sensations transmitted through the nerves that do not cause pain, trigger the nerves in the pain pathways.
Other Complications of Shingles
SECONDARY INFECTION: This can delay healing, and result in scarring. The scarred area sometimes remains numb. Scarring on the face can be disfiguring.
DISSEMINATION: Occasionally shingles may spread to other areas of the skin, or even to internal organs. This happens mostly in immunocompromised patients and can lead to serious consequences such as the development of pneumonia or encephalitis (an inflammation of the brain and its surrounding membranes.
RECURRENCE: If you have shingles once, for the most part, you will never get it again. This situation is different however in immunocompromised patients. Immunocompromised are those whose immune systems are weakened by a disease such as AIDS, by drugs used to suppress the rejection of a transplanted organ, or by radiation or chemotherapy for cancer. They are at increased risk of experiencing a recurrence. Recurrences are treated the same as primary attacks.
WHAT IS YOUR BIGGEST FRUSTRATION RIGHT NOW?
In spite of your best efforts you still cannot manage the constant pain. How often, do you hear yourself saying, “No, I have not tried a “free” sample of PainBreak yet; I’ve been meaning to.” Many are getting relief who thought they never could. Now it’s your turn.
Send for your “free” sample Today!
Remember, it is always wise to seek advice from your own health practitioner before making any major changes to your current course of treatment.
From Boyce Berkel, MD, PhD – Neuralgia Relief Center ~ For Your Health and Betterment.
Visit PainBreak.com